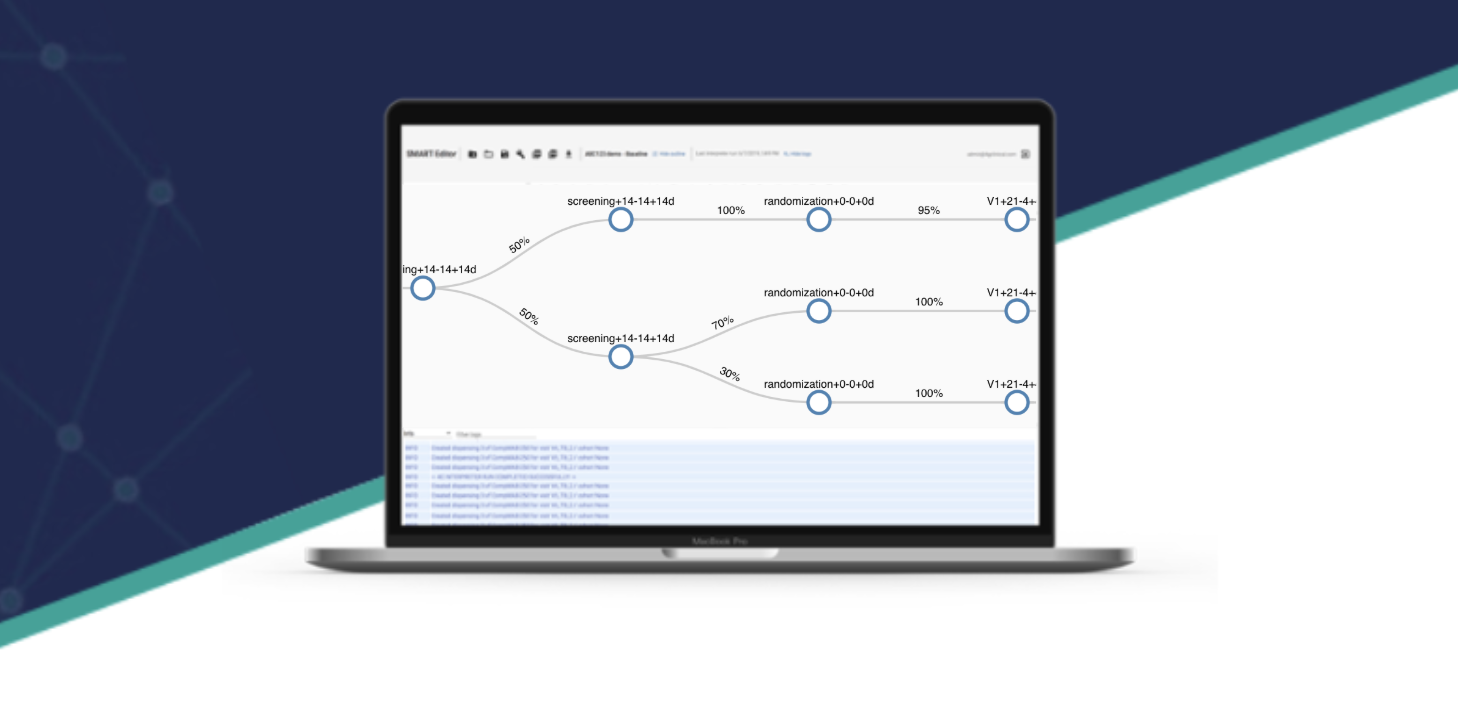
With all the focus on various electronic data capture (EDC) solutions in the clinical trials world over the past decade(s), few people seem to have noticed the exponential advances made in the real workhorse systems of the trials: randomization and trial supply management (RTSM). Also known as IVRS, IWRS and more commonly IRT, these interactive response technology systems have advanced to actually execute randomization, blinded supply and resupply management to depots and sites, and most importantly of all, drug dispensing. Is there anything more important to get right?
Yet RTSM continues to fly under the radar to a large extent, as we as an industry focus on shiny new clinical data management solutions, patient outcomes and enrollment forecasting technologies. Perhaps it’s time for that to change.
Let’s look back:
First generation: Patient-numbered kit labels
The first generation of RTSM technology consisted of patient-numbered kit labels, shipped to all sites in (generally) full blocks corresponding to the full course of treatments for a study. Emergency break blind was done with sealed envelopes. The sheer quantity of supply wasted in this method by non-enrolling sites, sites that didn’t fill up randomization blocks, and patient dropouts, was staggering. But at the time it was simply the cost of doing business. There was no other way.
Second generation: IVRS
Enter the first clinical Interactive Voice Response System (IVRS), developed in the 1990s in order to randomize patients over the phone, and later, to dispense drug and resupply sites as well. For the first time, all patient kits could be interchangeable for any other equivalent kit. Supply became much more flexible, and the supply for a dropped out patient could easily be used by a subsequent patient in the same treatment arm… and no one would be the wiser. Also, shipping no longer needed to occur in blocks, nor in full courses of treatment, so in a 2 TG 4 block size trial with 6 dispensing visits and 100 sites, you could start each site with, say, 2 kits (one A and one B) instead of 24 kits (full block of 6 visits * 4 TGs) for a total startup overage of 200 kits instead of 2400 kits, with significantly lower waste to boot. That’s dramatic.
In addition, IVRS allowed more complex trial designs to evolve. Nowadays we think of variable dosing, multi stratified trials as the norm, but before IVRS, even strata-based randomization was not feasible in multi-center trials.
Everyone went to IVRS, of course, for any significantly sized double blind clinical trials, and suddenly there was more supply than demand. The order of the day was for customers to write 200-300 page system specifications, which were then coded and later tested, over a roughly 12 week span from the time a sponsor said “Go” to the time the trial could actually go live. Three months. And that’s only if the sponsor thought of and described every single thing correctly in the specification- and nothing in the trial changed since then.
Third generation: IWR / IRT / Parameter Based
In the early 2000s, the first parameter-driven, web-based systems were born. These are actually two different innovations which occurred over the same span of time. The web-based innovation (called interactive web response [IWR] at the time) simply replaced onerous phone keypad work and associated errors with slick html screens to collect, organize and display data all at once. No one who used an IWR ever wanted to use IVRS again, and today it is generally agreed that 99% or more of all RTSM transactions go through the web rather than the phone. IVRS is, for all intents and purposes, dead.
But the real innovation of the 2000s was the notion of “parameter driven” RTSM. The idea was to replace the slow and error prone 12-week waterfall development method with a fast, screen-based “configuration.” In many cases, trials could be set up right out of the box by selecting or entering information about visit schedule, treatment arms, dosing, etc. One large pharmaceutical that I was involved with went live with such a system in 2001 and to this day has run 80%+ of all trials through that system.
More of these types of systems emerged through the end of the decade and into the 2010s, and it feels like (if you read the hype) by now, everyone either has or claims to have a configurable, or partly configurable system. And when true, that’s a good thing for everyone involved. We are, after all, trying to improve speed and efficiency of bringing new, lifesaving medicines to people who need them, and any valuable innovation should be appreciated by all.
Trial designers have not been idle, however. As pressures have increased on the biopharmaceutical world to operate more efficiently, the complexity of trial designs has grown exponentially. It’s almost as if, seeing the rise of configurable systems, the biopharma world said, “Oh yeah? Let’s see if you can handle this!” And then they kept saying that for about 5 or 10 years.
The result for 3rd generation RTSMs has been spiraling complexity and an endless chase after new features. Complex, semi-predictable dosing requires more complex, specialized resupply algorithms. (Not to mention pressure on drug supply in general.) Very few people understood these algorithms and their control switches back when they are simple. Now they have become a black art.
So, while 3rd generation RTSM is clearly superior to all that came before it, it is running into some pretty significant friction of its own. 2nd generation systems manifested their natural friction (endless timelines and repetitive busy work) in a pressure cooker work environment with no hope of a better day. 3rd generation systems seem to be developing their own pressure cooker: constant innovation to keep up with trial designs, spiraling complexity daunting away those same sorts of people who suffered in generation two.
So what is to be done? This is the core question that I hope to answer in the coming months and years. In short: I think our world may be ready for a new way of doing things.
Editor's Note: This blog post was published just as the company was founded. In October of 2016 4G Clinical launched Prancer, the 4th generation of RTSM. Our use of modern technologies in clinical trials delivers a fully cloud-based, 100% configurable RTSM using natural language processing.
.png?width=250&name=Read%20About%20The%204th%20Generation%20of%20IRT%20(1).png)